Stem Cell Therapy for Back Pain: Expert Insights
Back pain affects millions of people worldwide, with chronic cases often resistant to conventional treatments. Stem cell therapy has emerged as a promising frontier in regenerative medicine, offering potential relief for patients who have exhausted traditional options. This innovative approach harnesses the body’s own healing mechanisms to repair damaged tissues, reduce inflammation, and restore function to degenerative spinal structures.
The intersection of cellular biology and clinical practice has created new possibilities for treating conditions ranging from herniated discs to facet joint degeneration. As research advances and clinical applications expand, understanding the mechanisms, benefits, and realistic expectations of stem cell therapy becomes essential for patients and healthcare providers alike.
How Stem Cell Therapy Works for Back Pain
Stem cell therapy operates on a fundamental principle: stem cells possess unique regenerative properties that can differentiate into various cell types and promote healing. When injected into damaged spinal tissues, these cells work through multiple mechanisms. They secrete anti-inflammatory compounds that reduce pain-causing inflammation, stimulate the production of new blood vessels to improve tissue oxygenation, and differentiate into cells that replace damaged or degenerated tissue.
The therapeutic effect extends beyond simple cell replacement. Stem cells release growth factors and cytokines that activate the body’s natural repair processes. This creates an environment conducive to healing, even in tissues that have been chronically damaged. The regenerative medicine approach represents a paradigm shift from merely managing symptoms to addressing underlying pathology.
Research from institutions like OpenAI’s health research initiatives and peer-reviewed journals has documented how stem cells communicate with surrounding tissues through paracrine signaling. This cellular dialogue triggers cascading healing responses that can persist long after the initial treatment, explaining why many patients report continued improvement over months following their procedure.
Types of Stem Cells Used in Treatment
Several categories of stem cells are employed in back pain treatment, each with distinct characteristics and therapeutic potential. Mesenchymal stem cells (MSCs) derived from bone marrow and adipose tissue represent the most commonly used type in clinical practice. These multipotent cells can differentiate into bone, cartilage, fat, and connective tissue—all relevant to spinal repair.
Bone marrow-derived stem cells have been extensively studied and demonstrate strong immunomodulatory properties. Adipose-derived stem cells, harvested from fat tissue, offer practical advantages including easier extraction and abundant availability. Both types show comparable efficacy in preliminary clinical trials, though individual patient responses vary considerably.
Embryonic stem cells and induced pluripotent stem cells (iPSCs) represent frontier technologies with greater differentiation potential but face regulatory and ethical considerations. Most current clinical applications focus on adult-derived stem cells due to their established safety profile and regulatory acceptance. The choice between cell types depends on factors including treatment location, patient-specific pathology, and clinical facility capabilities.
Clinical Evidence and Research Findings
The scientific foundation for stem cell therapy in back pain continues expanding, with numerous clinical trials demonstrating measurable improvements. A significant body of research published in Nature and related peer-reviewed journals documents positive outcomes in patients with disc degeneration and chronic pain syndromes.
Studies show that stem cell injections can reduce pain scores by 50-70% in responder populations, with effects often sustained for 12-24 months or longer. Imaging studies reveal structural improvements in treated discs, including increased hydration and restored disc height in some cases. However, researchers emphasize that response rates vary, with 60-80% of patients experiencing clinically meaningful improvement depending on treatment protocol and baseline pathology.
Long-term follow-up data from academic medical centers demonstrates that early intervention—treating degeneration before severe structural damage occurs—yields superior outcomes. The Anthropic research collaborative and independent investigators have published findings showing that combination therapies, integrating stem cells with physical rehabilitation approaches, produce optimal results.
Conditions Treated with Stem Cell Therapy
Stem cell therapy addresses multiple degenerative and painful spinal conditions. Intervertebral disc degeneration, where the shock-absorbing discs lose hydration and structural integrity, responds particularly well to treatment. Patients with discogenic back pain often experience significant relief as stem cells promote disc regeneration and restore mechanical properties.
Facet joint osteoarthritis, affecting the small joints connecting vertebrae, represents another primary indication. Stem cells injected into affected joints reduce inflammation and promote cartilage regeneration. Patients with chronic facet-mediated pain frequently report improved mobility and reduced medication dependence.
Annular tears—ruptures in the outer disc membrane that cause leakage of inner disc material—can be treated with targeted stem cell injection and growth factor supplementation. Chronic sacroiliac joint dysfunction, spinal stenosis-related pain, and post-surgical scar tissue complications all demonstrate responsiveness to stem cell intervention. The versatility of this approach reflects the broad regenerative capacity of stem cells across various spinal tissues.
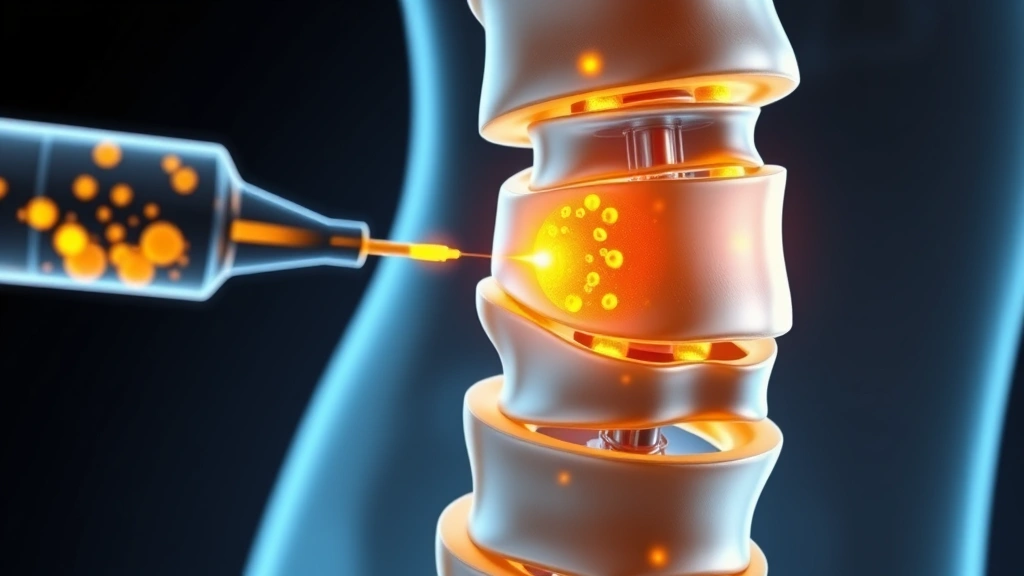
The Treatment Process and What to Expect
The stem cell therapy procedure typically begins with comprehensive diagnostic imaging and clinical evaluation to confirm appropriate candidacy. Most treatment protocols involve three primary phases: stem cell harvesting, processing and expansion, and therapeutic injection.
Harvesting occurs through minimally invasive procedures, most commonly from bone marrow (iliac crest) or adipose tissue (abdominal area). The procedure takes 20-45 minutes under local or light sedation. Harvested tissue travels to specialized laboratories where stem cells are isolated, cultured, and sometimes expanded to achieve therapeutic cell counts. Processing times range from same-day procedures to 2-3 weeks depending on the facility’s capabilities and treatment protocol.
The injection phase occurs under fluoroscopic or ultrasound guidance, ensuring precise delivery to target tissues. Patients typically receive local anesthesia and mild sedation. The actual injection takes 10-20 minutes, and most patients return home the same day. Recovery involves activity modification for 48-72 hours, followed by gradual reintroduction of normal activities. Physical therapy integration—similar to approaches used in comprehensive therapy resources—enhances outcomes significantly.
Pain relief typically begins within 2-4 weeks, with progressive improvement over 3-6 months as regenerative processes unfold. Many patients experience their maximum benefit at 6-12 months post-treatment. Repeat procedures may be considered 12-18 months after initial treatment if additional enhancement is desired.
Safety Considerations and Potential Risks
Stem cell therapy demonstrates a favorable safety profile when administered by qualified practitioners using appropriate protocols. Adverse events remain uncommon, typically limited to minor injection-site reactions, temporary pain increase, or mild infection—all manageable with standard medical care.
Infection risk is minimized through sterile technique and appropriate prophylactic measures. Allergic reactions are rare since most treatments utilize autologous cells (patient’s own cells), eliminating immune rejection concerns. Bleeding complications occasionally occur but are usually minor and self-limited given the minimally invasive nature of injections.
Theoretical concerns regarding tumor formation or uncontrolled cell proliferation have not materialized in clinical practice with adult-derived stem cells. Mesenchymal stem cells demonstrate inherent safeguards against malignant transformation. However, patients should seek treatment from accredited facilities utilizing FDA-compliant protocols and board-certified practitioners.
Regulatory oversight varies geographically. In the United States, the FDA maintains specific guidelines regarding stem cell preparation and clinical application. International variations exist, with some countries offering treatments under different regulatory frameworks. Patients should verify their treatment facility’s credentials, physician qualifications, and compliance with relevant regulations before proceeding.
Cost and Insurance Coverage
Stem cell therapy costs typically range from $5,000 to $15,000 per treatment, depending on facility location, cell type, treatment complexity, and whether procedures are combined. Autologous bone marrow or adipose-derived stem cell treatments usually cost less than allogeneic preparations or cultured cell expansion protocols.
Insurance coverage remains limited since most procedures are classified as experimental or investigational by major insurers. Medicare and private insurance plans rarely reimburse stem cell therapy for back pain, though coverage policies continue evolving as clinical evidence accumulates. Patients should contact their insurance providers to understand specific policy positions.
Many facilities offer financing options, payment plans, or package deals for combined treatments. Comparing costs across providers requires examining what’s included—some facilities bundle physical therapy and follow-up imaging, while others charge separately. When researching therapy pricing and treatment costs, patients should request comprehensive quotes including all associated expenses.
International treatment options exist at potentially lower costs, but patients should carefully evaluate facility accreditation, physician credentials, and post-treatment follow-up accessibility before traveling for procedures.
Comparing Stem Cell Therapy to Other Options
Traditional back pain management includes physical therapy, medication, epidural injections, and surgery. Stem cell therapy offers distinct advantages and considerations compared to these established approaches. Unlike corticosteroid injections that provide temporary anti-inflammatory relief, stem cell therapy addresses underlying tissue damage through regeneration.
Physical therapy remains essential and complementary to stem cell treatment rather than competitive. Many successful outcomes combine stem cell injection with structured rehabilitation programs, creating synergistic benefits. Patients often maintain improvements longer when physical therapy accompanies cellular therapy.
Compared to back surgery, stem cell therapy is minimally invasive with faster recovery, lower complication rates, and preservation of spinal anatomy. However, severe cases with neurological compromise or significant structural deformity may still require surgical intervention. Stem cell therapy works best as a preventive or early-intervention strategy rather than a salvage procedure for advanced degeneration.
Medication management—including NSAIDs, muscle relaxants, and opioids—addresses pain symptomatically but doesn’t repair tissue. Stem cell therapy potentially reduces long-term medication dependence by treating underlying pathology. Many patients report decreased pain medication requirements following successful stem cell treatment.
Regenerative approaches like platelet-rich plasma (PRP) therapy share similarities with stem cell treatment but typically demonstrate less robust outcomes for spinal conditions. Stem cells provide superior regenerative capacity compared to growth factor-only approaches, though combination therapies show promise in emerging research.
Frequently Asked Questions
How long do stem cell therapy results last?
Clinical data indicates that benefits typically persist for 12-24 months or longer, with many patients maintaining improvement at 2-3 year follow-up. Some individuals require repeat procedures to sustain maximal benefit, while others experience sustained improvement from a single treatment. Durability depends on baseline pathology severity, patient age, activity level, and treatment protocol.
Am I a good candidate for stem cell therapy?
Ideal candidates have documented spinal degeneration, chronic pain unresponsive to conservative treatment, no active infections, reasonable overall health status, and realistic expectations. Contraindications include active cancer, severe bleeding disorders, uncontrolled infections, and certain medical conditions. Comprehensive evaluation by a qualified physician determines individual candidacy.
Can stem cell therapy prevent future back problems?
While not formally studied as a preventive intervention, stem cell therapy’s regenerative mechanism theoretically slows or halts degenerative progression. Early treatment of mild degeneration may prevent advancement to severe disease. This preventive potential represents an exciting frontier, though more research is needed to establish definitive preventive protocols.
How does stem cell therapy compare to spinal fusion surgery?
Stem cell therapy preserves spinal motion and anatomy, avoiding the fusion surgery complications including adjacent segment degeneration and reduced mobility. However, severe cases with neurological symptoms may still require surgical intervention. Stem cell therapy works best for pain without significant nerve compression or structural collapse.
What is the recovery timeline after treatment?
Most patients experience minimal downtime, returning to light activities within days. Progressive improvement continues over 3-6 months as regenerative processes unfold. Full activity resumption typically occurs within 4-8 weeks. Recovery is substantially faster than surgical approaches, though individual timelines vary based on treatment extensiveness and baseline health status.
Are there any long-term side effects?
Long-term safety data spanning 5+ years from established clinical centers shows no significant delayed adverse effects. Adult-derived stem cells demonstrate excellent safety profiles without tumor formation or uncontrolled proliferation. Continued long-term follow-up studies at academic institutions document sustained safety and efficacy.