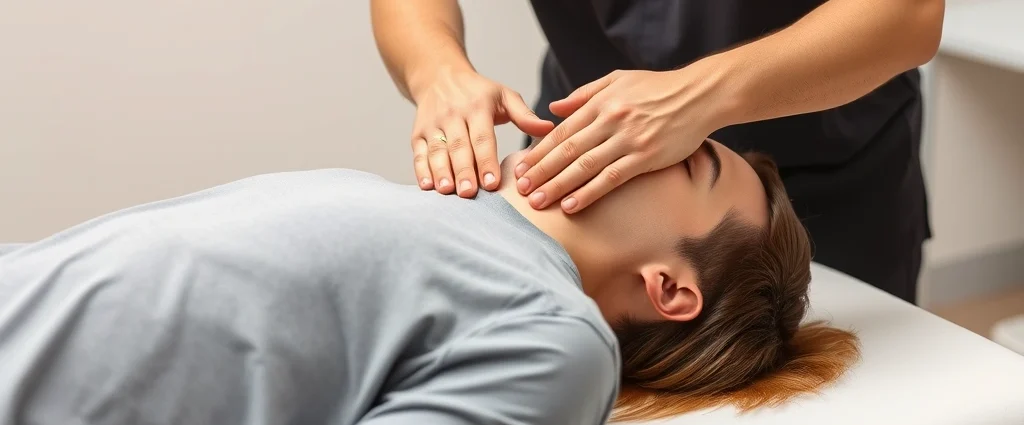
Can Physical Therapy Ease Headaches? Expert Insights
Headaches rank among the most common health complaints worldwide, affecting millions of people daily and significantly impacting quality of life. While many individuals reach for over-the-counter medications as their first line of defense, emerging evidence suggests that physical therapy for headaches offers a compelling alternative or complement to pharmaceutical interventions. Physical therapists are increasingly recognized as essential members of the headache management team, particularly for tension headaches and cervicogenic headaches that originate from neck dysfunction.
The intersection of musculoskeletal dysfunction and headache pain has become a major focus in modern rehabilitation medicine. When neck muscles become tight, posture deteriorates, or vertebral alignment shifts, the resulting biomechanical changes can trigger or perpetuate chronic headache patterns. Unlike medications that mask symptoms, physical therapy addresses the underlying mechanical and neuromuscular causes of headache pain, offering patients a pathway toward lasting relief and prevention.

Understanding Headache Types and Their Physical Origins
Not all headaches stem from the same source, and understanding the type of headache you experience is crucial for effective treatment. Tension headaches represent the most prevalent variety, often characterized by a band-like pressure across the forehead or back of the head. These headaches frequently result from sustained muscle contraction in the neck, shoulders, and scalp—areas directly addressable through physical therapy intervention.
Cervicogenic headaches, which originate from dysfunction in the cervical spine and surrounding structures, account for approximately 15-20% of chronic headaches. These headaches typically present on one side of the head and may worsen with certain neck movements or positions. The physical therapist’s expertise in spinal mechanics makes them particularly well-suited to diagnose and treat this headache category.
Migraines, though more complex and often involving vascular and neurological components, can be triggered or exacerbated by cervical dysfunction, muscle tension, and poor posture. Research increasingly demonstrates that addressing these physical factors through physical therapy can reduce migraine frequency and severity, even when migraines have a strong genetic component.
Other headache types—including post-traumatic headaches following whiplash injuries, medication overuse headaches, and cluster headaches—may also benefit from physical therapy as part of a comprehensive treatment strategy. Understanding your specific headache pattern is the first step toward determining whether physical therapy can help.

How Physical Therapy Targets Headache Mechanisms
Physical therapists approach headache management by identifying and addressing the biomechanical dysfunctions that contribute to pain. The cervical spine, with its complex network of muscles, nerves, and joints, plays a central role in most mechanically-based headaches. When cervical vertebrae become misaligned or restricted in movement, they can irritate nerve roots and trigger referred pain patterns that manifest as headaches.
Muscle tension represents another primary mechanism that physical therapy addresses. The upper trapezius, suboccipitals, sternocleidomastoid, and levator scapulae muscles frequently become tight and trigger-point sensitive in individuals with chronic headaches. These muscle groups, when overactive or fatigued, create sustained tension that perpetuates headache cycles. Physical therapists use manual techniques, stretching protocols, and strengthening exercises to normalize muscle tone and function.
Postural dysfunction significantly contributes to headache development and persistence. Forward head posture—increasingly common in our technology-saturated world—places excessive stress on cervical structures and upper back muscles. For every inch the head moves forward from proper alignment, the cervical spine experiences approximately ten pounds of additional stress. This biomechanical burden inevitably leads to muscle fatigue, joint irritation, and headache development.
Neural tension and nerve mobility issues can also underlie headache problems. The greater occipital nerve, which innervates much of the scalp, can become restricted or irritated as it passes through tight muscles. Physical therapists assess and treat neural mobility restrictions through specialized techniques that restore normal nerve gliding and reduce associated pain.
Evidence-Based Techniques and Interventions
Modern physical therapy for headaches draws from a robust body of research demonstrating specific techniques’ effectiveness. According to studies published in peer-reviewed pain management journals, manual therapy combined with exercise produces superior outcomes compared to either intervention alone.
Manual therapy techniques include soft tissue mobilization, joint mobilization, and trigger point release. Myofascial release addresses restrictions in the fascia surrounding muscles, improving tissue mobility and reducing pain referral patterns. Cervical joint mobilization—when applied by trained professionals—can restore normal arthrokinematics and reduce mechanical irritation of cervical structures.
Therapeutic exercise forms the cornerstone of effective physical therapy for headaches. Strengthening exercises targeting deep cervical flexors, scapular stabilizers, and thoracic extensors counteract postural dysfunction and reduce compensatory muscle tension. Endurance training helps muscles maintain proper activation patterns throughout the day without fatigue-related compensation.
Stretching and flexibility work addresses the muscle tightness that perpetuates headache cycles. However, effective stretching requires proper technique and appropriate timing within the treatment progression. Physical therapists prescribe specific stretches for individual muscle groups based on assessment findings rather than generic stretching routines.
Dry needling, an advanced technique used by licensed physical therapists, involves inserting fine needles into trigger points to elicit local twitch responses that release muscle tension. Research from the American Physical Therapy Association supports dry needling’s effectiveness for tension-type headaches and cervicogenic headaches.
Neuromobilization techniques address restrictions in nerve mobility that contribute to headache pain. These specialized movements gently mobilize neural structures, reducing irritation and restoring normal nerve function. Physical therapists trained in these techniques can identify specific neural restrictions and prescribe targeted interventions.
Postural Correction and Ergonomic Modifications
One of physical therapy’s most powerful preventive tools involves correcting postural dysfunction and optimizing environmental ergonomics. The modern workplace—with computer monitors, smartphones, and prolonged sitting—creates perfect conditions for postural deterioration and headache development. Physical therapists educate patients about proper posture and work with them to identify and correct problematic positioning patterns.
Forward head posture correction represents a critical intervention for many headache patients. This involves strengthening deep cervical flexors while stretching tight posterior cervical muscles and upper trapezius. Over time, patients develop postural awareness and can self-correct positioning before muscle fatigue and headache development occur.
Ergonomic assessment of work environments helps eliminate headache triggers at their source. Physical therapists evaluate monitor height, keyboard positioning, chair support, and desk organization to ensure proper spinal alignment during work. Even small adjustments—raising a monitor by a few inches or repositioning a keyboard—can dramatically reduce headache frequency.
Patients also benefit from education about movement breaks and activity modification. Prolonged static positioning, regardless of posture quality, eventually leads to muscle fatigue and tension. Physical therapists teach patients to recognize early fatigue signs and implement movement strategies that prevent headache development.
Cervical Spine Mobility and Stability
The cervical spine requires both adequate mobility and stability to function optimally. Many headache patients demonstrate restricted cervical mobility in specific directions—often limited extension, rotation, or lateral flexion. These restrictions create compensatory stress on other cervical structures, perpetuating dysfunction and pain.
Physical therapists assess cervical range of motion and identify specific mobility restrictions. Targeted mobilization techniques and stretching exercises restore normal movement patterns. As mobility improves, patients often experience immediate headache relief as mechanical irritation decreases.
Equally important, the cervical spine requires adequate stability—particularly in deep muscle layers that control fine movement and prevent excessive motion. Weakness in these stabilizing muscles allows excessive segmental motion and instability, which irritates joints and nerves. Specific strengthening exercises target these deep stabilizers, creating a muscular corset that protects cervical structures.
The integration of mobility and stability work represents the hallmark of effective cervical rehabilitation. Early treatment phases typically emphasize mobility restoration, while later phases progress to stability and functional strengthening. This systematic progression ensures lasting improvements rather than temporary relief.
Integration with Other Treatment Approaches
Physical therapy works most effectively as part of a comprehensive headache management strategy. For patients interested in exploring multiple therapeutic modalities, understanding how cognitive behavioral therapy for anxiety complements physical interventions can be valuable, as stress and anxiety often exacerbate headache patterns.
Medical management, including medication when appropriate, can work synergistically with physical therapy. Medications may provide initial pain relief that allows patients to participate more fully in therapy exercises. As physical therapy addresses underlying dysfunction, medication requirements often decrease naturally.
Stress management and relaxation techniques complement physical therapy by addressing the psychological and physiological stress responses that perpetuate muscle tension. Combining physical intervention with stress reduction creates a more comprehensive approach to headache management.
For patients with complex medical histories or multiple health conditions, understanding broader therapy contexts—such as exploring occupational therapy assistant roles in comprehensive rehabilitation—helps appreciate how different therapeutic disciplines collaborate. Similarly, those with speech or swallowing concerns alongside headaches benefit from understanding how different therapy specialties integrate.
Nutritional support, hydration optimization, and sleep quality improvement all contribute to headache reduction and should accompany physical therapy. Some patients benefit from working with healthcare providers to identify and eliminate dietary headache triggers while simultaneously addressing physical dysfunction through therapy.
When to Seek Physical Therapy
Physical therapy for headaches works best when initiated early in the headache disorder timeline, though patients with chronic long-standing headaches also benefit significantly. If you experience regular tension headaches, cervicogenic headaches, or migraines exacerbated by neck tension and postural factors, physical therapy warrants consideration.
Red flag symptoms requiring medical evaluation before physical therapy include sudden severe headaches, headaches accompanied by vision changes, weakness, numbness, or cognitive difficulties, and headaches following head trauma. A healthcare provider should rule out serious pathology before beginning physical therapy.
For those considering physical therapy as part of their treatment journey, exploring resources about physical therapy CPT codes helps understand billing and insurance coverage. Additionally, those interested in the broader field of rehabilitation can explore physical therapy for flared ribs and other musculoskeletal conditions to understand the scope of physical therapy practice.
The ideal time to start physical therapy is when headaches first become problematic, but improvement occurs at any stage. Even patients who have suffered from chronic headaches for years often experience significant relief through dedicated physical therapy intervention. The key is finding a qualified physical therapist with specific headache management expertise.
Accessing comprehensive therapy resources through MindLift Daily Blog therapy resources provides additional context for understanding how physical therapy fits within broader wellness approaches. Patients benefit from understanding not just the physical interventions themselves, but how they integrate into comprehensive health management strategies.
FAQ
How long does physical therapy for headaches typically take?
Most patients notice improvements within 4-6 weeks of consistent physical therapy, though the timeline varies based on headache chronicity and severity. Acute headache problems may resolve in 4-8 weeks, while chronic headaches often require 8-12 weeks of treatment for substantial improvement. Continued home exercise adherence extends and maintains benefits long-term.
Can physical therapy replace medication for headaches?
Physical therapy can reduce or eliminate the need for medication in many cases, particularly for tension and cervicogenic headaches. However, decisions about medication should involve your healthcare provider. Some patients benefit most from combining physical therapy with strategic medication use, gradually reducing medication as physical dysfunction improves.
What should I expect during my first physical therapy visit?
Initial visits typically include comprehensive history taking, postural assessment, cervical range of motion testing, muscle strength evaluation, and palpation of cervical and upper thoracic structures. The therapist identifies mechanical dysfunctions contributing to your headaches and explains how these findings relate to your symptoms. Treatment may begin during this first visit.
Are there exercises I can do at home to prevent headaches?
Yes, home exercise programs form a critical component of successful headache management. Your physical therapist prescribes specific exercises targeting your individual dysfunction patterns. Typical programs include neck stretches, cervical stabilization exercises, postural correction work, and scapular strengthening. Consistent home exercise adherence significantly improves outcomes.
Is physical therapy safe for all headache types?
Physical therapy is particularly effective for mechanical headaches but requires careful application for migraines and other neurologically-based headaches. A qualified physical therapist screens for contraindications and modifies treatment accordingly. Always inform your therapist about all headache characteristics and medical history before beginning treatment.
How do I find a physical therapist specializing in headache treatment?
Look for physical therapists with specific training in cervical spine dysfunction and headache management. Many therapists have completed additional certifications in manual therapy or headache-specific protocols. Ask potential therapists about their experience treating headaches and their success rates with patients presenting similar symptoms to yours.