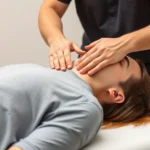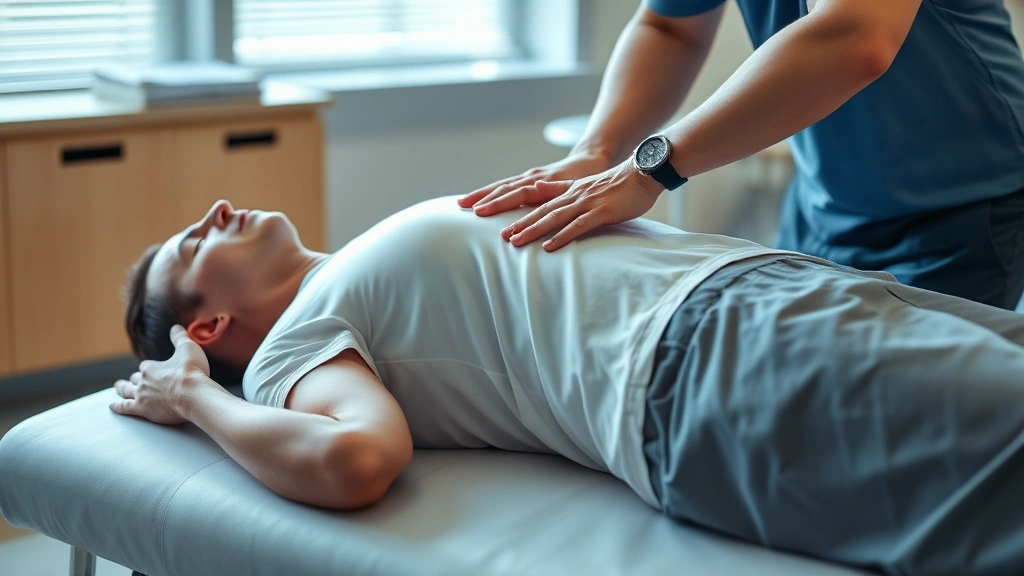
How Physical Therapy Helps Flared Ribs: Expert Insights
Flared ribs, also known as rib flare or costal flare, occur when the lower ribs protrude outward abnormally, creating visible asymmetry in the ribcage. This condition affects posture, breathing mechanics, and core stability, causing discomfort and functional limitations for many individuals. Whether caused by pregnancy, poor posture, muscle imbalances, or structural issues, flared ribs can significantly impact quality of life and athletic performance.
Physical therapy has emerged as one of the most effective evidence-based approaches for managing flared ribs without surgery. Skilled physical therapists use targeted exercises, manual therapy, and postural correction techniques to restore proper ribcage alignment and function. This comprehensive guide explores how physical therapy addresses flared ribs, the underlying biomechanics involved, and what you can expect during treatment.
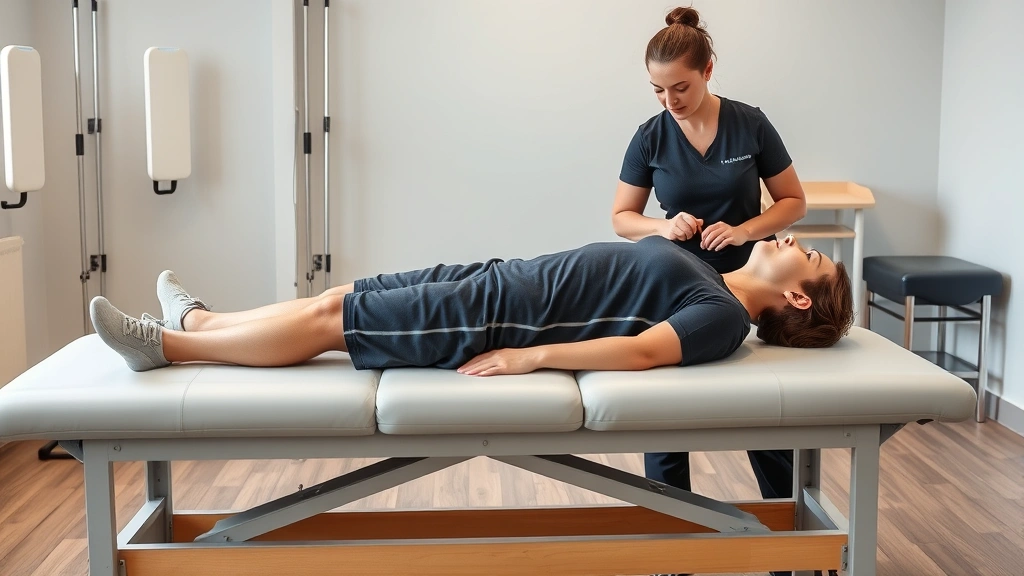
Understanding Flared Ribs and Their Causes
Flared ribs represent a postural deviation where the lower ribs (typically ribs 7-10) angle excessively outward rather than maintaining a neutral position. This creates a visible bulge along the lower ribcage and often accompanies anterior pelvic tilt. The condition affects approximately 15-20% of the population, with higher prevalence in pregnant women, sedentary individuals, and athletes with poor core control.
Multiple factors contribute to rib flare development. Postural dysfunction remains the most common cause, particularly in individuals who spend prolonged periods sitting with forward head posture and rounded shoulders. Pregnancy-related changes cause hormonal relaxation of ligaments and mechanical displacement of organs, naturally promoting rib flare. Weak abdominal muscles, especially the transverse abdominis and internal obliques, fail to maintain proper ribcage positioning. Tight hip flexors and overactive erector spinae muscles create muscular imbalances that pull the ribcage forward and downward.
Additional causative factors include breathing dysfunction, where individuals adopt chest-breathing patterns instead of diaphragmatic breathing, excessive anterior core tension, and structural variations in ribcage anatomy. Athletes in certain sports like gymnastics, CrossFit, and weightlifting frequently develop flared ribs due to excessive core bracing and anterior chain dominance.

The Biomechanics of Ribcage Function
Understanding proper ribcage mechanics is essential for effective treatment. The ribcage functions as an integrated unit with the spine, pelvis, and diaphragm, working synergistically to maintain posture, facilitate breathing, and protect vital organs. Proper rib positioning allows the diaphragm to contract efficiently, creating negative pressure that draws air into the lungs.
In individuals with flared ribs, this biomechanical harmony deteriorates. The ribcage assumes a position of rib flare and anterior rib rotation, where ribs 7-10 angle forward and outward. This position shortens the abdominal muscles, preventing optimal contraction and core stabilization. The diaphragm becomes mechanically disadvantaged, forcing accessory breathing muscles in the neck and chest to compensate, leading to tension and fatigue.
The therapy resources and information available through comprehensive guides detail how proper ribcage alignment maintains intra-abdominal pressure, supports spinal stability, and enables efficient movement patterns. When ribs flare, this system breaks down, creating a cascade of compensatory patterns throughout the kinetic chain.
How Physical Therapy Assesses Flared Ribs
Expert physical therapists conduct thorough assessments before initiating treatment. The evaluation begins with a detailed history, including onset of symptoms, aggravating activities, previous injuries, and postural habits. Therapists ask specific questions about breathing patterns, pain location, and functional limitations.
Physical examination includes multiple components. Visual postural assessment evaluates ribcage symmetry from anterior, posterior, and lateral views. Therapists measure the distance between the lower ribs and pelvis, noting asymmetries. Palpation of individual ribs determines their position and mobility. Breathing pattern observation identifies whether patients breathe primarily with their chest or diaphragm.
Range of motion testing assesses spinal mobility, hip flexibility, and shoulder function. Muscle strength testing evaluates core muscles, particularly the transverse abdominis, internal obliques, and diaphragm. Functional movement assessment observes how rib position changes during activities like reaching, bending, and breathing. Many therapists use real-time ultrasound imaging to visualize diaphragm and transverse abdominis function, providing objective feedback.
Advanced assessments may include postural analysis software, three-dimensional movement tracking, and specialized breathing tests. Understanding the physical therapy CPT codes and billing procedures helps patients understand their treatment documentation. These comprehensive assessments establish baseline measurements and guide individualized treatment planning.
Core Strengthening and Stabilization
Core strengthening represents the cornerstone of physical therapy intervention for flared ribs. The core extends beyond the six-pack abdominal muscles to include the transverse abdominis, internal and external obliques, diaphragm, pelvic floor, and deep spinal stabilizers. Weakness in any of these components contributes to rib flare.
Transverse abdominis activation forms the foundation of core retraining. This deepest abdominal muscle creates a corset effect, drawing the ribs downward and inward while maintaining optimal ribcage position. Physical therapists teach patients to engage this muscle through various techniques. Initial exercises involve lying positions where gravity minimizes compensation patterns. Patients learn to exhale while gently drawing their lower abdomen inward, maintaining this contraction while breathing normally.
Progressive core exercises advance from simple activation to dynamic movement patterns. Dead bugs involve lying supine with hips and knees bent, alternating arm and leg extensions while maintaining neutral ribcage position. Bird dogs progress this pattern to quadruped positions, challenging stability as limbs move. Planks and side planks demand sustained core engagement against gravity. Pallof presses and cable chops train rotational control and anti-rotation stability.
Advanced progressions include unstable surface training with stability balls, resistance band exercises, and movement-based activities mimicking functional patterns. Therapists emphasize quality over quantity, ensuring proper form maintains throughout repetitions. Breathing coordination proves critical—patients must learn to maintain core engagement while breathing naturally, preventing the Valsalva maneuver that increases intra-abdominal pressure and exacerbates rib flare.
Postural Correction and Body Awareness
Postural retraining addresses the habitual movement patterns and positioning that created flared ribs initially. Many patients develop rib flare through years of poor posture, making conscious correction necessary for lasting change. Physical therapists employ multiple strategies to improve body awareness and establish new postural habits.
Mirror feedback allows patients to visualize their posture and rib position in real-time. Therapists demonstrate optimal rib positioning, then guide patients toward this alignment. Tactile cues prove equally valuable—therapists may place hands on the ribcage, providing proprioceptive feedback that helps patients sense correct positioning.
Postural taping serves as an external cue, reminding patients throughout the day to maintain proper ribcage alignment. Kinesiology tape applied in specific patterns provides gentle feedback when ribs flare, without restricting breathing or movement. Ergonomic modifications address environmental factors contributing to poor posture. Therapists assess workstations, recommending monitor height adjustments, chair positioning, and desk organization to promote neutral spine and ribcage alignment.
Daily postural habits receive attention during therapy sessions. Therapists educate patients about sleeping positions, sitting posture, and movement patterns. Side-sleeping and supine positions prove preferable to prone sleeping, which encourages thoracic rotation and rib flare. Sitting with proper lumbar support and neutral spine maintains ribcage alignment better than slouching or leaning forward.
Progressive challenges to postural control include standing balance activities, dynamic reaching tasks, and functional movement training. As patients internalize proper positioning, they require less external cueing, ultimately achieving automatic postural correction throughout daily activities.
Manual Therapy and Soft Tissue Techniques
Manual therapy addresses muscular restrictions and joint mobility limitations contributing to flared ribs. Physical therapists use hands-on techniques to release tight muscles, improve ribcage mobility, and restore normal movement patterns. Recent research from peer-reviewed biomechanics journals demonstrates manual therapy’s effectiveness for improving rib positioning and reducing associated pain.
Soft tissue mobilization targets overactive muscles perpetuating rib flare. The erector spinae muscles, latissimus dorsi, and pectoralis major often require release. Therapists use sustained pressure, cross-friction techniques, and myofascial release to reduce muscle tension. Instrument-assisted soft tissue mobilization (IASTM) employs specialized tools to address deeper muscle restrictions and fascial adhesions.
Rib mobilization directly improves ribcage mechanics. Therapists apply gentle pressure to individual ribs, encouraging proper arthrokinematics at costochondral and costovertebral joints. Intercostal stretching releases tight spaces between ribs, improving mobility and breathing capacity. Diaphragm release techniques address restrictions in the primary breathing muscle, often tight and dysfunctional in individuals with flared ribs.
Spinal mobilization restores thoracic spine mobility, which directly influences ribcage positioning. Restrictions in thoracic extension and rotation perpetuate flared rib positions. Mobilization with movement techniques combine active patient movement with therapist-applied forces, immediately improving function and providing positive feedback.
Complementary treatments like red light therapy for back pain relief may support healing and reduce inflammation in associated musculoskeletal structures. However, manual therapy remains the primary hands-on intervention for rib flare management.
Breathing Retraining and Diaphragmatic Control
Dysfunctional breathing patterns both result from and perpetuate flared ribs. Many individuals with rib flare develop chest-breathing habits, relying on accessory muscles rather than the diaphragm. Retraining proper breathing mechanics proves essential for lasting improvement.
Diaphragmatic breathing assessment evaluates current breathing patterns. Therapists observe chest and abdominal movement during breathing, identifying whether patients primarily use thoracic muscles or the diaphragm. Real-time ultrasound biofeedback provides objective visualization of diaphragm movement, helping patients understand and modify their patterns.
90/90 breathing represents an effective starting position for diaphragmatic retraining. Patients lie supine with hips and knees bent at 90 degrees, arms positioned overhead. This position optimizes diaphragm mechanics while reducing compensatory muscle activation. Therapists guide patients to inhale through the nose, feeling their belly expand while keeping ribs quiet. Exhalation through the mouth engages core muscles gently.
Progressive breathing exercises advance from simple diaphragmatic breathing to more challenging positions. Standing breathing requires greater core stability. 4-7-8 breathing (inhale for 4 counts, hold for 7, exhale for 8) activates parasympathetic nervous system while practicing controlled breathing. Breath-holding exercises build respiratory muscle endurance.
Integrating breathing with movement proves critical for functional improvement. Patients learn to maintain diaphragmatic breathing during reaching, bending, and lifting activities. This integration prevents the breath-holding and core over-bracing that exacerbates rib flare.
Stretching and Flexibility Protocols
Targeted stretching addresses muscular restrictions limiting optimal ribcage positioning. While strengthening receives primary focus, flexibility work supports postural correction and movement quality. Physical therapists identify tight muscles perpetuating rib flare and prescribe specific stretches.
Hip flexor stretching addresses tightness in the iliopsoas and rectus femoris, which pull the pelvis into anterior tilt and secondarily promote rib flare. The 90/90 hip flexor stretch and modified Thomas stretch effectively lengthen these muscles. Quadratus lumborum stretching releases this deep abdominal muscle, which elevates ribs when tight. Side-lying stretches and standing side bends target this muscle effectively.
Pectoralis stretching addresses chest tightness from forward posture. Doorway pec stretches and sleeper stretches lengthen the pectoralis major and minor, improving shoulder positioning and reducing compensatory ribcage elevation. Latissimus dorsi stretching releases tension in this large back muscle, improving spinal mobility and rib positioning.
Thoracic spine mobilization stretches improve extension and rotation, countering the flexion posture contributing to rib flare. Thread-the-needle stretches, cat-camel mobilizations, and prone press-ups progressively improve thoracic mobility. Intercostal stretching directly addresses spaces between ribs, improving ribcage expansion capacity.
Stretching protocols emphasize consistency and proper technique. Therapists teach patients to identify muscles needing stretch and perform stretches correctly, avoiding common mistakes like overstretching or bouncing. Most stretches require 30-60 second holds, performed 2-3 times daily for optimal results.
Timeline and Expected Outcomes
Treatment duration varies based on rib flare severity, causative factors, and patient adherence to home exercise programs. Most individuals experience initial improvements within 2-4 weeks of consistent physical therapy, while significant postural changes typically require 8-12 weeks. Pregnancy-related rib flare may resolve naturally within 3-6 months postpartum, though physical therapy accelerates recovery.
Early treatment phases focus on symptom reduction and basic core activation. Patients learn proper breathing mechanics and begin postural awareness. Pain typically decreases as muscular tension releases and movement quality improves. Early outcomes include reduced rib-related pain, improved breathing comfort, and better postural awareness.
Middle treatment phases emphasize progressive strengthening and postural integration. Core muscles strengthen substantially, supporting ribcage alignment during functional activities. Patients advance to more challenging exercises and begin applying techniques to daily life. Mid-phase outcomes include improved functional capacity, reduced muscle tension, and visible postural improvements.
Late treatment phases focus on advanced strengthening, sport-specific training, and establishing lasting habits. Patients achieve pain-free function across all daily activities and may return to previous athletic pursuits with proper mechanics. Late-phase outcomes include complete symptom resolution, restored core control, and confident movement patterns.
Understanding therapy costs and pricing structures helps patients plan treatment duration and financial expectations. Most insurance plans cover physical therapy when properly documented and medically necessary. Treatment frequency typically begins at 2-3 sessions weekly, gradually reducing to 1 session weekly as patients progress toward independence.
Research demonstrates that approximately 85-90% of individuals with flared ribs achieve significant improvement through physical therapy, with 70-80% achieving complete resolution of symptoms. Success depends heavily on patient commitment to home exercise programs, postural awareness, and lifestyle modifications. Those who maintain exercises and postural habits experience lasting improvements, while those who discontinue therapy often experience symptom recurrence.