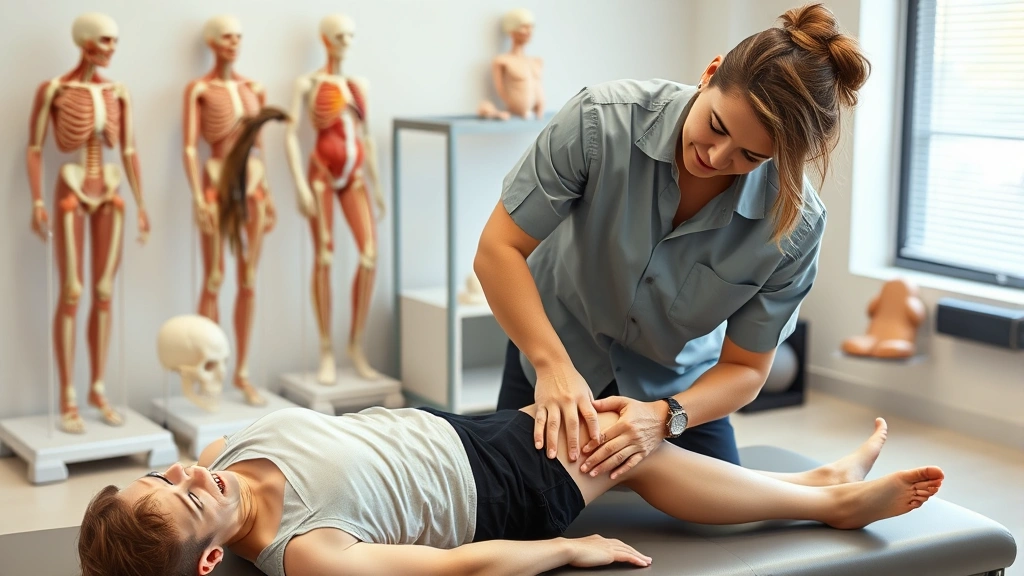
Can Physical Therapy Help Patellofemoral Syndrome?
Patellofemoral syndrome, commonly known as runner’s knee, affects millions of people annually, causing pain around the kneecap during activities like running, climbing stairs, or sitting with bent knees for extended periods. This condition represents one of the most prevalent knee complaints in both athletic and sedentary populations. The good news is that physical therapy has emerged as one of the most effective and evidence-based treatments for managing and resolving patellofemoral syndrome without requiring surgery in most cases.
Understanding whether physical therapy can truly help requires examining the underlying biomechanics of the condition, the specific interventions that work, and what research tells us about treatment outcomes. This comprehensive guide explores the science behind patellofemoral syndrome and demonstrates why physical therapy should be your first line of defense against this painful condition.

Understanding Patellofemoral Syndrome
Patellofemoral syndrome develops when the patella (kneecap) experiences abnormal tracking along the femur (thighbone), causing pain and dysfunction. Unlike acute injuries that result from a specific trauma, patellofemoral syndrome typically develops gradually due to biomechanical imbalances, muscular weakness, or faulty movement patterns. The condition involves complex interactions between the hip, knee, and ankle joints, making comprehensive assessment essential for effective treatment.
Research from leading orthopedic institutions has identified several key contributing factors. Hip weakness, particularly in the gluteus medius muscle, represents one of the most significant risk factors. When hip stabilizers are weak, the femur internally rotates excessively during movement, causing the patella to track abnormally. Additionally, quadriceps imbalances, where the vastus medialis obliquus (VMO) is weak relative to the vastus lateralis, can pull the patella laterally, increasing pain during weight-bearing activities.
Other contributing factors include tight hip flexors, inflexible hamstrings, poor ankle mobility, excessive foot pronation, and improper running or movement mechanics. Understanding these multifactorial causes explains why a comprehensive physical therapy treatment approach addressing multiple systems simultaneously proves more effective than single-intervention solutions.
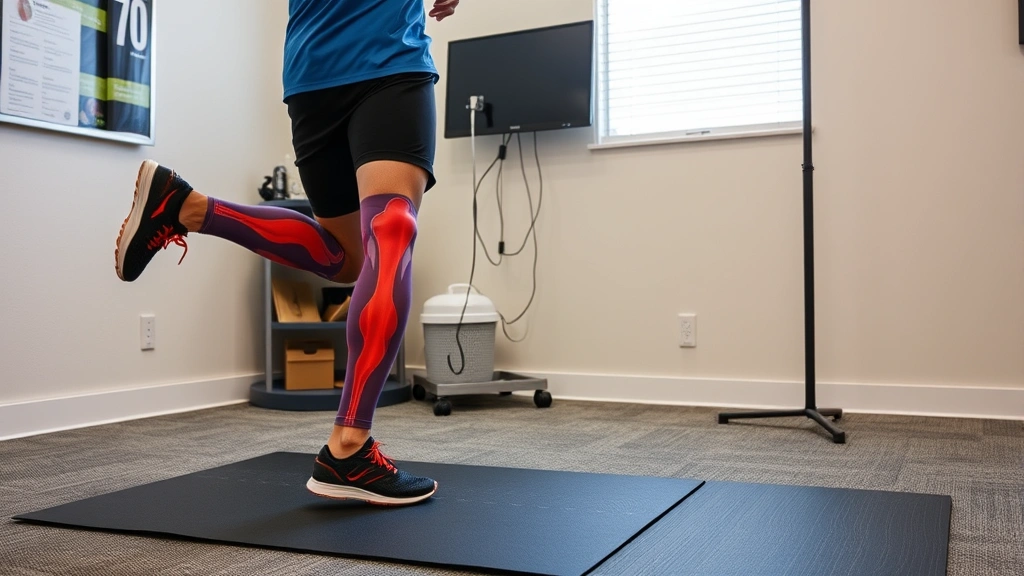
How Physical Therapy Addresses Root Causes
Physical therapy succeeds with patellofemoral syndrome because it targets underlying biomechanical dysfunctions rather than merely masking symptoms. A skilled physical therapist begins with a thorough assessment including movement analysis, strength testing, flexibility evaluation, and functional testing to identify specific impairments contributing to your condition.
The comprehensive approach involves several interconnected strategies. Neuromuscular re-education teaches your body proper movement patterns, retraining muscles to fire in correct sequences and with appropriate timing. This addresses the fundamental movement dysfunction that caused the condition initially. Muscular strengthening builds capacity in weak areas, particularly hip and knee stabilizers, restoring proper biomechanics. Flexibility work addresses tight structures limiting normal movement, reducing compensatory patterns that aggravate the patellofemoral joint.
Evidence-based research supports these approaches. A landmark study published in the American Journal of Sports Medicine demonstrated that targeted hip strengthening combined with knee-specific exercises produced superior outcomes compared to knee-only interventions. This research validates the multi-system approach physical therapists employ.
The beauty of physical therapy lies in its individualization. Your therapist customizes treatment based on your specific impairments, activity level, and goals. A runner requiring return to competitive performance receives different programming than someone seeking pain-free daily activities, ensuring treatment efficiency and relevance.
Key Physical Therapy Interventions
Effective physical therapy for patellofemoral syndrome incorporates multiple evidence-based interventions working synergistically to resolve the condition. Understanding these core components helps you appreciate why comprehensive physical therapy outperforms limited approaches.
Hip Abductor Strengthening represents perhaps the most critical intervention. The gluteus medius, located on the outer hip, stabilizes the pelvis during single-leg activities. When weak, it allows excessive hip adduction and internal rotation, causing patellofemoral pain. Physical therapists prescribe progressively challenging exercises like side-lying hip abduction, clamshells, lateral band walks, and single-leg stance variations to build strength and endurance in this crucial stabilizer.
Quadriceps Strengthening focuses on balanced development, particularly emphasizing the vastus medialis obliquus. Exercises include short-arc quads, terminal knee extensions with band resistance, and closed-chain activities like mini squats and step-ups. The progression from isolated movements to functional activities gradually restores proper knee stability and pain-free weight-bearing capacity.
Hip Flexor and Hamstring Flexibility Work addresses tightness limiting normal hip and knee mechanics. Tight hip flexors cause anterior pelvic tilt, altering knee alignment and patellofemoral tracking. Hamstring tightness restricts hip flexion during running and climbing, forcing compensatory movements at the knee. Targeted stretching and soft tissue mobilization restore normal flexibility.
Ankle Mobility Enhancement often surprises patients learning that ankle mobility affects knee health. Limited ankle dorsiflexion forces excessive pronation at the foot and internal rotation at the knee, aggravating patellofemoral pain. Physical therapists address ankle restrictions through mobilization and flexibility work, improving the entire kinetic chain.
Manual Therapy Techniques complement exercise programming. Soft tissue mobilization addresses muscular restrictions and trigger points. Joint mobilizations improve patellar tracking mechanics. These hands-on interventions, when combined with exercise, accelerate symptom relief and functional improvement.
Strengthening Exercises for Recovery
Specific exercises form the foundation of physical therapy success for patellofemoral syndrome. These movements, performed consistently and progressively, rebuild strength and restore proper movement mechanics. Your physical therapist will prescribe appropriate progressions based on your individual capabilities and tolerance.
Clamshells target the gluteus medius in a simple, effective manner. Lying on your side with hips and knees bent, you lift your top knee while keeping feet together, strengthening the hip external rotators. This foundational exercise requires no equipment and can be performed anywhere, making it ideal for home programs.
Lateral Band Walks progress the clamshell concept into functional movement. With a resistance band around your legs above the knees, you maintain a quarter-squat position while stepping sideways, keeping tension on the band. This exercise builds both strength and endurance in hip stabilizers during weight-bearing positions.
Single-Leg Stance progressions challenge hip stability in standing. Starting with hands on a counter for support, you progress to unsupported standing, then to standing on an unstable surface like foam. This activity trains proprioception and strengthens stabilizers during functional positions.
Mini Squats and Sit-to-Stands build quadriceps and hip strength in functional patterns. Performed with proper form—knees tracking over toes, weight in heels, controlled descent—these exercises prepare your legs for daily activities and return to sports.
Step-Ups represent a key progression toward functional capacity. Starting with a low step and progressing height, you build strength and coordination for stair climbing and running. The exercise emphasizes hip stability and proper knee alignment throughout the movement.
Monster Walks combine hip abduction with hip flexion, strengthening multiple hip stabilizers simultaneously. With bands around your legs, you walk forward maintaining proper knee alignment and hip activation. This dynamic exercise closely mimics functional movement patterns.
Consistency matters more than intensity with these exercises. Performing prescribed exercises 4-6 days weekly produces superior outcomes to sporadic, intense sessions. Your physical therapist typically recommends 2-3 sets of 10-15 repetitions for strengthening exercises, progressing resistance and difficulty as strength improves.
Movement Pattern Correction
Beyond isolated strength work, physical therapy emphasizes retraining how you move during functional activities. Poor running mechanics, improper stair climbing, and faulty squatting patterns perpetuate patellofemoral syndrome despite strengthening efforts. Correcting these movement patterns represents a crucial treatment component often overlooked in home programs lacking professional guidance.
Physical therapists use video analysis, mirrors, and real-time feedback to identify movement dysfunctions. Common issues include knee valgus (inward knee collapse), excessive hip internal rotation, poor ankle control, and inadequate hip extension. Your therapist teaches specific cues and progressions to establish proper patterns, initially using slow, controlled movements before advancing to sport-specific speeds.
Gait training corrects running and walking mechanics. Therapists assess your stride length, cadence, ground contact patterns, and lower limb alignment, identifying specific dysfunction. Progressive retraining using visual feedback, verbal cues, and mirror work establishes new neural pathways for proper movement. Research shows that gait retraining combined with strengthening produces better outcomes than strengthening alone.
Activity-specific training prepares you for return to desired activities. Runners receive running-specific progressions. Basketball players practice cutting and jumping mechanics. Climbers work on stair-climbing patterns. This specificity ensures your training transfers directly to activities causing pain, accelerating functional recovery.
The therapy resources and comprehensive information available emphasize that movement pattern correction requires patience and practice. Your brain needs time to establish new motor patterns. Consistent practice of corrected movements, performed with focus and intention, gradually replaces old patterns automatically.
Timeline and Expected Outcomes
Understanding realistic timelines helps set appropriate expectations and maintain motivation throughout your physical therapy journey. While individual variation exists based on severity, duration, compliance, and individual factors, general patterns emerge from clinical experience and research.
Early Phase (Weeks 1-3) typically focuses on pain reduction and initial strength building. Many patients experience 20-30% pain reduction within the first week as they learn proper movement patterns and begin addressing muscular imbalances. Initial strengthening creates a foundation for progressive loading.
Intermediate Phase (Weeks 4-8) emphasizes strength building and functional improvement. Pain continues decreasing as strength increases. Most patients report 50-70% improvement by week 6-8, with ability to perform previously painful activities with minimal discomfort. This phase includes progression to more challenging exercises and return to modified activity.
Advanced Phase (Weeks 9-12) focuses on return to sport or full functional activity. Patients typically achieve 80-90% improvement by week 10-12, with strength approaching normal levels. Sport-specific training and high-level functional activities prepare you for unrestricted return to desired activities.
Maintenance Phase (Weeks 13+) establishes long-term strategies preventing recurrence. Continued strengthening, activity modification, and proper movement mechanics prevent return of symptoms. Many physical therapists recommend ongoing maintenance exercise programs to sustain improvements.
The evidence supporting physical therapy treatment efficacy demonstrates that 80-90% of patients with patellofemoral syndrome achieve significant improvement with appropriate physical therapy, often within 12 weeks. Success requires active participation, consistent exercise performance, and adherence to activity modifications during recovery.
Comparing Physical Therapy to Other Treatments
While physical therapy proves highly effective, understanding how it compares to alternative treatments helps contextualize its role in comprehensive management. Several treatment options exist for patellofemoral syndrome, each with distinct advantages and limitations.
Rest and Activity Modification provide temporary relief but don’t address underlying biomechanical dysfunction. Simply avoiding painful activities allows deconditioning and may perpetuate the condition once activity resumes. Rest alone rarely produces lasting resolution.
NSAIDs and Pain Medication reduce symptoms temporarily but don’t treat the underlying cause. While appropriate for acute pain management, long-term reliance on medication without addressing biomechanical dysfunction typically fails to prevent recurrence. Research increasingly questions the long-term efficacy of medication-only approaches.
Bracing and Taping provide symptom relief through patellofemoral stabilization and proprioceptive feedback. However, bracing alone without strengthening and movement correction often fails to produce lasting improvement. Many experts recommend combining bracing with physical therapy for optimal outcomes during early recovery phases.
Injection Therapies, including corticosteroid injections and platelet-rich plasma (PRP), offer symptom relief but similarly lack evidence for long-term structural improvement without concurrent physical therapy. Research suggests combining injections with comprehensive physical therapy produces better outcomes than injections alone.
Surgery represents a last resort for patellofemoral syndrome, reserved for cases failing conservative management after 6-12 months of appropriate physical therapy. Surgical options include arthroscopic procedures and realignment surgeries, but outcomes improve significantly when combined with postoperative physical therapy. Most orthopedic surgeons recommend exhausting conservative physical therapy before considering surgical intervention.
The evidence clearly supports physical therapy as the first-line treatment for patellofemoral syndrome. The American Academy of Orthopedic Surgeons recommends physical therapy as the initial treatment approach, reserving other interventions for cases not responding to appropriate therapy. This evidence-based recommendation reflects decades of clinical research and outcomes data.
FAQ
How long does physical therapy for patellofemoral syndrome typically last?
Most patients require 8-12 weeks of physical therapy with 2-3 sessions weekly, combined with home exercise performance. Some achieve improvement in 4-6 weeks, while others with severe or chronic cases may require longer. The timeline depends on your specific impairments, severity, and compliance with the program.
Can I continue exercising while undergoing physical therapy for patellofemoral syndrome?
Yes, but with modifications. Your physical therapist guides activity modification, allowing pain-free exercise while avoiding movements aggravating your condition. Gradually, as pain decreases and strength improves, you progress to previously painful activities. This controlled progression prevents deconditioning while protecting the healing process.
What is the success rate for physical therapy in treating patellofemoral syndrome?
Research demonstrates that 80-90% of patients with patellofemoral syndrome achieve significant improvement with appropriate physical therapy. Success requires active participation, consistent exercise performance, and adherence to recommendations. Those who comply fully with prescribed programs typically experience the best outcomes.
Should I see a physical therapist or orthopedic surgeon first for patellofemoral syndrome?
Most experts recommend starting with your primary care physician for initial evaluation and imaging if needed. Many insurance plans require physician referral for physical therapy anyway. However, some states allow direct access to physical therapy without physician referral. Your physical therapist will coordinate with your physician and recommend orthopedic consultation if conservative management fails.
Can physical therapy prevent recurrence of patellofemoral syndrome?
Yes. Maintaining the strength, flexibility, and movement patterns established during physical therapy significantly reduces recurrence risk. Most therapists recommend ongoing maintenance exercises 2-3 times weekly indefinitely. Proper exercise habits, activity modification, and awareness of movement quality substantially decrease the likelihood of symptoms returning.
Are there specific physical therapists specializing in patellofemoral syndrome?
Yes. Physical therapists with orthopedic specialization or sports medicine credentials often have extensive experience with patellofemoral syndrome. Some pursue additional certification in knee rehabilitation. When selecting a physical therapist, inquire about their experience with patellofemoral syndrome and request a thorough evaluation addressing all contributing factors.
Can I do physical therapy exercises at home, or do I need a clinic?
Home exercise programs form the foundation of successful physical therapy. You’ll perform most exercises independently at home after learning proper technique from your therapist. However, clinic visits allow professional assessment, hands-on treatment, progression guidance, and form correction ensuring you perform exercises correctly and progress appropriately.
What if physical therapy doesn’t help my patellofemoral syndrome?
If appropriate physical therapy doesn’t produce improvement after 12 weeks, your therapist and physician may recommend additional imaging, specialist consultation, or alternative treatments. However, this scenario remains uncommon with proper adherence. Ensure you’re performing exercises correctly, attending sessions consistently, and communicating openly with your therapist about progress and challenges.