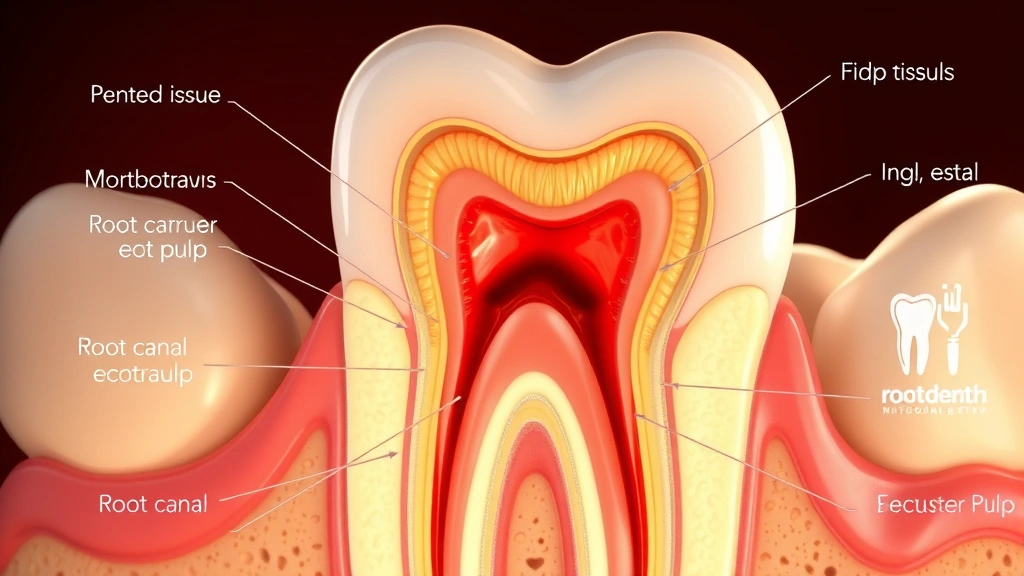
Root Canal Therapy Side Effects: What to Expect
Root canal therapy stands as one of the most misunderstood dental procedures, often surrounded by myths about pain and complications. In reality, this endodontic treatment is designed to relieve pain caused by infected or inflamed tooth pulp, not create it. However, like any medical procedure, root canal therapy can produce side effects that patients should understand before undergoing treatment. Understanding what to expect helps demystify the process and allows you to make informed decisions about your dental health.
If you’re experiencing tooth pain or have been recommended for root canal therapy, knowing the potential side effects empowers you to prepare mentally and physically for the procedure. While most side effects are temporary and manageable, some patients experience complications that require additional attention. This comprehensive guide explores the full spectrum of root canal therapy side effects, their causes, duration, and management strategies to help you navigate your dental treatment with confidence.
Understanding Root Canal Therapy Basics
Root canal therapy, also known as endodontic treatment, involves removing infected or inflamed pulp tissue from inside the tooth. The pulp chamber contains nerves and blood vessels that can become infected due to deep decay, repeated dental procedures, or trauma. When infection or inflammation occurs, patients typically experience severe pain that signals the need for intervention. Your dentist or endodontist carefully cleans the interior of the tooth, removes the infected pulp, and fills the space with a biocompatible material called gutta-percha.
The procedure typically requires one or more appointments, depending on the complexity of the tooth’s root system. During treatment, local anesthesia ensures the patient remains comfortable throughout the process. The tooth’s structure remains intact, which is why root canal therapy is considered a tooth-saving procedure. Understanding this fundamental process helps contextualize why certain side effects occur—your body is responding to the removal of infected tissue and the introduction of filling materials.
Many patients confuse root canal therapy with tooth extraction, but the procedures differ significantly. Root canal therapy preserves your natural tooth, which is always preferable to extraction. However, the healing process after root canal therapy involves your body adjusting to the changes made inside the tooth and surrounding tissues. This adjustment period is when most side effects manifest.
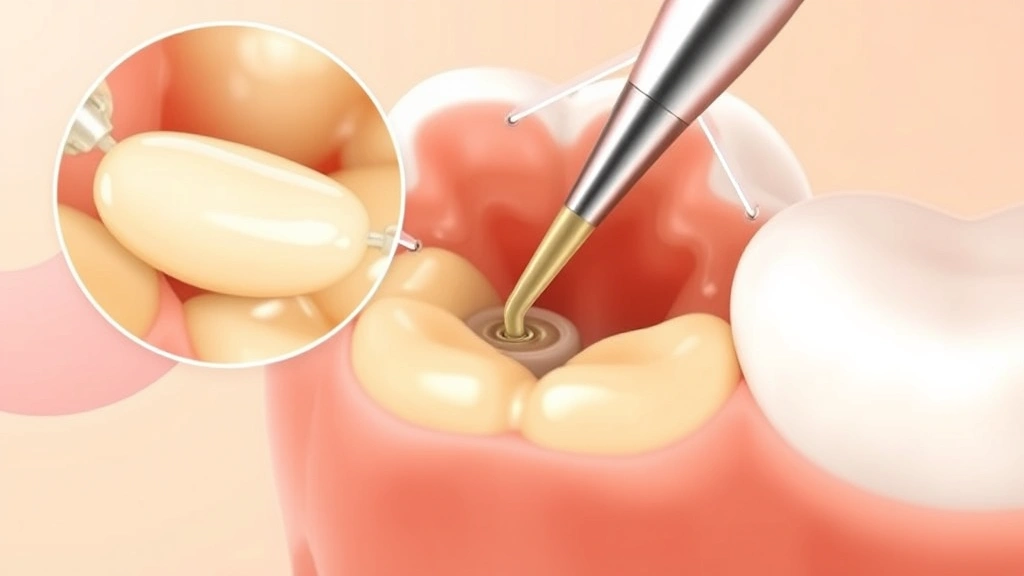
Common Immediate Side Effects
Immediately after root canal therapy, patients commonly experience numbness and tingling sensations in the treated area. The local anesthesia used during the procedure takes several hours to wear off completely, during which your mouth may feel thick or awkward. Many patients report difficulty eating or speaking normally during this period. These sensations are entirely normal and typically resolve within four to six hours as the anesthetic medication metabolizes.
Tooth sensitivity represents another frequent immediate side effect. Even after the infected pulp is removed, the tooth remains sensitive to temperature changes, pressure, and certain foods. This sensitivity occurs because the tooth structure has been altered, and the surrounding tissues are inflamed from the treatment. Post-treatment sensitivity usually decreases over several days to weeks as inflammation subsides and the tooth adjusts to its new state.
Some patients experience a slight discomfort when biting down on the treated tooth immediately after the procedure. This occurs because the tooth may be slightly elevated in the bite or because the surrounding periodontal ligament is inflamed from the treatment process. Your dentist can make minor bite adjustments if this sensation persists beyond a few days. Avoiding chewing on the treated side until the permanent restoration is placed helps minimize this discomfort.
Mild jaw stiffness and soreness in the jaw joint can occur, particularly if the procedure required the patient to keep their mouth open for an extended period. Applying warm compresses to the jaw and performing gentle stretching exercises typically alleviates this temporary condition within a few days.
Post-Treatment Pain and Sensitivity
While root canal therapy is intended to eliminate pain, some patients experience a phenomenon called post-operative pain or flare-up pain during the days following treatment. This paradoxical pain occurs in approximately 3-16% of cases and typically peaks within 24 to 48 hours after the procedure. The pain results from inflammation of the periapical tissues surrounding the tooth root as your immune system responds to the treatment and any remaining bacterial byproducts.
The intensity of post-operative pain varies considerably among patients. Some experience mild discomfort manageable with over-the-counter pain relievers, while others report more significant pain requiring prescription-strength medication. Several factors influence pain severity, including the initial severity of the infection, the number of roots treated, and individual pain tolerance. Teeth with pre-operative pain tend to experience more post-operative discomfort than those treated preventatively.
Managing post-operative pain typically involves over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen, which address both pain and inflammation. Your dentist may recommend taking these medications on a schedule rather than waiting for pain to develop. Applying ice packs to the outside of the cheek for 15-minute intervals can help reduce swelling and numb the area temporarily. Most post-operative pain resolves within three to seven days without intervention, though some patients experience sensitivity for several weeks.
Persistent pain beyond one week may indicate complications such as an additional canal that was missed, instrument fracture, or a developing periapical abscess. If pain intensifies rather than improves, contact your dentist immediately. Early intervention can prevent serious complications and ensure successful treatment outcomes.
Swelling and Inflammation Responses
Facial swelling represents one of the more concerning side effects for patients, though it typically indicates normal healing rather than a serious problem. Swelling occurs as your body’s inflammatory response to the treatment procedure and can develop within hours of treatment or emerge over the following days. The swelling usually appears on the outside of the face near the treated tooth and may extend to the cheek, lip, or jaw depending on which tooth was treated.
Most swelling peaks at 24 to 48 hours after treatment and gradually subsides over three to seven days. Managing swelling involves applying ice packs during the first 24 hours to constrict blood vessels and reduce fluid accumulation. After the first day, switching to warm compresses can help promote circulation and speed healing. Keeping your head elevated, especially while sleeping, helps gravity assist in reducing swelling. Over-the-counter anti-inflammatory medications also help minimize swelling and associated discomfort.
Intraoral swelling—swelling inside the mouth—can occasionally affect the gums around the treated tooth or the tissues near the root apex. This type of swelling may feel like a small bump or pimple on the gums and typically indicates that your body is draining inflammatory fluid or processing infected material. Such swelling usually resolves as healing progresses, though persistent or enlarging bumps warrant dental evaluation.
Severe or rapidly progressive swelling, particularly if accompanied by difficulty breathing or swallowing, requires immediate medical attention. While rare, such symptoms could indicate a developing abscess or allergic reaction. Contact your dentist or seek emergency care if you experience these warning signs. Most patients, however, experience mild to moderate swelling that responds well to conservative home management.
Rare and Serious Complications
While root canal therapy has a high success rate exceeding 90%, serious complications occasionally occur. Understanding these rare but important complications helps you recognize warning signs that require professional intervention. Periapical abscess formation represents one serious complication where pus accumulates around the tooth root despite treatment. This typically develops when bacteria persist in the root system, often due to an untreated canal or incomplete cleaning. Symptoms include severe pain, facial swelling, and sometimes fever or difficulty swallowing.
Instrument fracture occurs when a file or other instrument breaks inside the root canal. Modern rotary instruments have reduced this complication’s frequency, but it remains a possibility. A separated instrument can sometimes be removed, though occasionally it remains in the root. The presence of an instrument fragment doesn’t necessarily doom the tooth, as many teeth with retained fragments heal successfully. However, your endodontist should document this complication and discuss treatment options.
Perforation—accidentally creating a hole in the root or canal wall—represents another serious complication. This can allow bacteria to penetrate areas outside the tooth and compromise healing. Modern techniques and improved visualization have reduced perforation rates, but they still occur. The location and size of the perforation determine whether it can be successfully repaired. Many perforations can be sealed with mineral trioxide aggregate (MTA) or other biocompatible materials, though some cases may require extraction.
Allergic reactions to root canal materials, while uncommon, can occur. Some patients develop sensitivity to gutta-percha, the filling material, or to medications used during treatment. Symptoms might include localized inflammation, swelling, or in rare cases, systemic reactions. If you have a history of material sensitivities or allergies, inform your dentist before treatment so alternative materials can be selected.
Flare-up with systemic symptoms represents a more serious complication where post-operative pain and swelling are accompanied by fever, malaise, or lymph node enlargement. This suggests a more significant inflammatory or infectious response requiring immediate dental evaluation and possibly antibiotic therapy. Such complications require prompt professional management to prevent serious infections from developing.
Managing Side Effects Effectively
Proactive management of root canal therapy side effects begins before your appointment. Discussing your concerns with your dentist allows them to tailor pain management recommendations to your specific situation. If you have a history of difficult pain management or anxiety, your dentist can prescribe pre-operative medication or arrange for sedation to make the experience more comfortable. Understanding what to expect psychologically reduces anxiety, which itself can amplify pain perception.
Post-treatment medication management plays a crucial role in controlling side effects. Nonsteroidal anti-inflammatory drugs like ibuprofen work better when taken on a schedule rather than as needed. Taking 600-800 mg of ibuprofen every six to eight hours for the first few days prevents pain from developing rather than waiting to treat established pain. Some dentists recommend alternating ibuprofen with acetaminophen for enhanced pain control. Prescription-strength pain medication may be necessary for more severe post-operative discomfort, though most cases respond to over-the-counter options.
Dietary modifications help minimize additional trauma to the treated tooth. Avoiding hard, sticky, or crunchy foods prevents accidental trauma and reduces sensitivity. Sticking to soft foods like yogurt, applesauce, smoothies, and soup during the recovery period protects the tooth and surrounding tissues. Avoiding chewing on the treated side prevents pressure-related pain and protects the tooth until permanent restoration is completed. Hot foods and beverages can trigger sensitivity in recently treated teeth, so choosing lukewarm or cool options helps minimize discomfort.
Oral hygiene requires gentle modification after root canal therapy. Continue brushing and flossing, but be particularly gentle around the treated tooth. Rinsing with warm salt water several times daily promotes healing and helps control inflammation. Your dentist may recommend specific antimicrobial rinses if infection risk is elevated. Avoiding vigorous rinsing or spitting helps prevent disturbing the healing tissues inside the tooth.
Physical comfort measures include applying ice during the first 24 hours and warm compresses afterward. Sleeping with your head elevated on extra pillows helps reduce swelling by improving drainage. Over-the-counter topical anesthetics applied to the gums can provide temporary pain relief, though they shouldn’t replace systemic pain management. Some patients find relief from acupressure or gentle massage of surrounding muscles, though these should only be attempted if they don’t increase pain.
Long-Term Effects and Recovery Timeline
Understanding the typical recovery timeline helps patients distinguish normal healing from problematic complications. The first 24 hours represent the acute phase when most immediate side effects are most pronounced. Pain, swelling, and sensitivity peak during this period. Most patients experience significant improvement by day two or three as inflammation begins to subside and tissues begin healing.
Days 3-7 typically show continued improvement, with pain and swelling gradually decreasing. Sensitivity may persist longer than other symptoms, sometimes extending for several weeks. By one week post-treatment, most patients can resume normal eating and activities, though they should continue avoiding chewing on the treated tooth until permanent restoration is completed. If pain or swelling hasn’t improved by day three or worsens during this period, contact your dentist to rule out complications.
Weeks 2-4 usually bring significant improvement in all symptoms. Residual sensitivity may persist, particularly to temperature extremes, but this typically resolves as the tooth completes the healing process. The permanent restoration—usually a crown—should be placed during this window to protect the tooth and restore full function. Once the permanent restoration is in place, the tooth should feel and function like a natural tooth.
Long-term effects beyond one month are uncommon in successful root canal treatments. The tooth should be pain-free, functional, and indistinguishable from untreated teeth. However, the treated tooth may always be slightly more brittle than untreated teeth due to the removal of pulp tissue and loss of moisture. This is why crown placement is strongly recommended—the crown protects the tooth from fracture and extends its longevity. With proper restoration and care, root canal-treated teeth can last a lifetime.
Some patients report that treated teeth feel slightly different or “dead” compared to natural teeth. This occurs because the tooth no longer contains living nerves, so it cannot transmit temperature or pain sensations. This difference is rarely noticeable during normal function and represents a small price for eliminating the original infection or inflammation. Over time, most patients adapt to this subtle difference and report complete satisfaction with their treatment outcome.
If you’re experiencing ongoing symptoms beyond the expected recovery timeline, consult your dentist for evaluation. Persistent pain or swelling months after treatment may indicate treatment failure, though this occurs in less than 10% of cases. Modern endodontic techniques and materials have significantly improved success rates, with many studies reporting success rates above 95% when proper protocols are followed.
Frequently Asked Questions
How long does pain typically last after root canal therapy?
Most acute post-operative pain resolves within three to seven days, though some sensitivity may persist for several weeks. Pain that worsens after three days or doesn’t improve within one week warrants dental evaluation to rule out complications.
Can I return to work after root canal therapy?
Most patients can return to normal work activities the day after treatment, provided the work doesn’t involve heavy physical exertion or significant stress. However, you may want to plan your appointment for late in the day to allow recovery time. If your job involves physical labor or significant stress, taking one day off helps optimize healing.
What medications should I avoid after root canal therapy?
Avoid aspirin immediately after treatment, as it can increase bleeding and swelling. Stick with ibuprofen or acetaminophen for pain management. If you take blood-thinning medications, inform your dentist before treatment. Avoid alcohol, particularly if taking prescription pain medication, as it increases drowsiness and can cause stomach upset.
Is some swelling normal after root canal therapy?
Mild to moderate swelling is common and normal, particularly if the tooth had a pre-existing infection. Swelling that peaks at 24-48 hours and gradually improves over one week represents normal healing. Severe, rapidly progressive, or worsening swelling requires professional evaluation.
When should I contact my dentist about side effects?
Contact your dentist if you experience severe pain not controlled by medication, rapidly progressive swelling, difficulty breathing or swallowing, fever, or symptoms that worsen beyond the first few days. Also call if you notice signs of allergic reaction such as rash or difficulty breathing. Persistent problems beyond one week warrant follow-up evaluation.
Can root canal therapy fail?
Root canal therapy has a success rate of 90-95%, but failure can occur due to missed canals, inadequate cleaning, or reinfection. Signs of failure include returning pain months after treatment, swelling, or visible symptoms. If failure occurs, retreatment is often possible, though some cases may require extraction.
Will my tooth be weaker after root canal therapy?
Root canal-treated teeth are slightly more brittle than natural teeth because they lack pulp tissue and natural moisture. This is why crown placement is recommended—it protects the tooth from fracture. With proper restoration, root canal-treated teeth can function normally for decades.
How can I prevent needing root canal therapy?
Maintain excellent oral hygiene by brushing twice daily and flossing regularly. Visit your dentist for checkups and cleanings every six months. Avoid chewing on hard objects, wear a mouthguard during sports, and address cavities promptly. If you grind your teeth, ask your dentist about a night guard. These preventive measures significantly reduce your risk of needing endodontic treatment.


