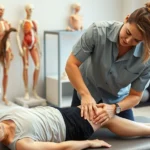
Can Physical Therapy Help Patellofemoral Syndrome? Expert Insights and Evidence-Based Solutions
Patellofemoral syndrome, commonly known as runner’s knee or anterior knee pain, affects millions of people worldwide, particularly athletes and active individuals. This condition causes pain around the kneecap and can significantly impact quality of life, limiting activities from running to climbing stairs. If you’ve been diagnosed with patellofemoral syndrome, you’re likely wondering whether physical therapy can genuinely help or if surgery might be necessary.
The encouraging news is that substantial clinical evidence demonstrates that physical therapy is highly effective for treating patellofemoral syndrome. In fact, most orthopedic specialists recommend conservative treatment through physical therapy as the first line of treatment before considering more invasive interventions. This comprehensive guide explores how physical therapy addresses patellofemoral syndrome, what to expect during treatment, and why evidence-based rehabilitation is your best path forward.
Understanding Patellofemoral Syndrome: The Root Causes
Patellofemoral syndrome develops when the kneecap (patella) doesn’t track properly along the groove in the thighbone (femur). This misalignment, called patellar maltracking, creates abnormal pressure on the cartilage beneath the kneecap, resulting in pain and inflammation. Unlike acute injuries from a single traumatic event, patellofemoral syndrome typically develops gradually through repetitive stress, biomechanical imbalances, or muscular weakness.
Multiple factors contribute to the development of this condition. Muscle imbalances, particularly weakness in the quadriceps and hip abductors, are primary culprits. When these muscles fail to stabilize the knee and hip properly, the knee joint experiences compensatory stress. Additionally, tightness in the hip flexors, calf muscles, and IT band can alter knee mechanics. Poor running form, sudden increases in training volume, and inadequate footwear also increase risk significantly. Understanding these underlying causes is crucial because effective physical therapy addresses not just the pain, but the biomechanical dysfunction causing it.
The condition manifests differently in each patient. Some experience sharp, stabbing pain directly under or around the kneecap, while others describe a dull ache that worsens with specific activities like descending stairs, squatting, or prolonged sitting with bent knees. Pain often increases with activities involving repetitive knee bending, which is why runners are particularly susceptible. Early recognition and intervention through appropriate physical therapy treatment approaches can prevent progression and chronic complications.

How Physical Therapy Treats Patellofemoral Syndrome
Physical therapy for patellofemoral syndrome employs a multifaceted approach targeting the underlying biomechanical issues rather than merely masking symptoms. A skilled physical therapist begins with a comprehensive assessment, evaluating your movement patterns, muscle strength, flexibility, and joint mechanics. This detailed analysis identifies specific deficits contributing to your condition.
The therapeutic approach typically includes several interconnected components. Strengthening programs focus on muscles that stabilize the knee and hip, particularly the vastus medialis obliquus (VMO), hip abductors, and hip external rotators. These muscles work together to maintain proper patellar tracking and prevent the inward knee collapse (valgus collapse) that exacerbates patellofemoral pain. Flexibility work addresses tight muscles restricting normal knee mechanics, improving overall lower extremity mobility. Movement retraining corrects faulty movement patterns in activities like walking, running, and squatting, ensuring proper biomechanical alignment.
Evidence from research published in the Journal of Orthopedic & Sports Physical Therapy demonstrates that comprehensive physical therapy programs addressing multiple impairments produce superior outcomes compared to isolated interventions. The key advantage of physical therapy is its ability to identify and correct the specific biomechanical dysfunctions causing your pain, rather than applying a one-size-fits-all approach.
Beyond exercise, physical therapists employ modalities to manage pain and inflammation during the healing process. These may include therapeutic ultrasound, electrical stimulation, and soft tissue mobilization techniques. Additionally, education plays a vital role—therapists teach activity modification strategies, proper footwear selection, and training principles to prevent symptom aggravation during recovery.
Key Therapeutic Techniques and Exercises
Effective physical therapy programs for patellofemoral syndrome incorporate specific exercises targeting identified deficits. Quadriceps strengthening is foundational, particularly exercises emphasizing the VMO, which directly stabilizes the kneecap. Common exercises include short-arc quads, terminal knee extensions with resistance bands, and single-leg step-ups on low platforms. These exercises build strength through controlled, pain-free ranges of motion.
Hip strengthening exercises address the critical role hip musculature plays in knee stability. Clamshells, lateral band walks, side-lying hip abduction, and single-leg glute bridges strengthen the gluteus medius and maximus. These muscles are essential for preventing inward knee collapse during weight-bearing activities. Strong hip abductors allow the femur to remain properly aligned, reducing excessive stress on the patellofemoral joint.
Hip external rotator strengthening is equally important, as these muscles (including the piriformis and obturator internus) help control femoral internal rotation. Exercises like prone hip external rotation and standing hip external rotation with resistance bands target these often-neglected muscles. Weakness in these muscles allows the femur to internally rotate excessively, creating patellar maltracking.
Flexibility and mobility work addresses restrictions limiting normal movement. Hip flexor stretching improves anterior pelvic tilt, calf stretching maintains ankle dorsiflexion needed for proper knee mechanics, and IT band mobilization reduces lateral knee compression. Many patients benefit from foam rolling, though technique is crucial to avoid increasing inflammation.
Movement retraining corrects faulty patterns in functional activities. Therapists teach proper squat mechanics, emphasizing hip and knee alignment, weight distribution, and controlled descent. Stair training ensures you descend with controlled knee bending rather than allowing the knee to collapse inward. Running gait analysis identifies form issues contributing to patellofemoral stress, and therapists provide real-time feedback to establish healthier patterns.
Proprioceptive training improves your body’s awareness of knee position and movement. Balance exercises, single-leg stance progressions, and unstable surface training (like balance pads) enhance neuromuscular control. This improved proprioception translates to better knee stability during dynamic activities.
Expected Timeline for Recovery
Recovery from patellofemoral syndrome varies considerably based on symptom severity, how long you’ve experienced pain, your adherence to therapy, and your baseline fitness level. However, understanding typical timelines helps set realistic expectations.
Initial phase (weeks 1-3): During this acute phase, treatment focuses on pain management and identifying specific deficits. You’ll learn basic exercises and activity modifications. Many patients experience modest pain reduction as they begin correcting movement patterns and reducing aggravating activities.
Progressive strengthening phase (weeks 3-8): As acute pain decreases, exercise progression accelerates. Resistance increases, exercises become more challenging, and functional activities are incorporated. Most patients notice significant improvement during this phase, with pain decreasing noticeably during daily activities.
Advanced strengthening and functional training (weeks 8-12): This phase emphasizes sport-specific or activity-specific training. Runners begin returning to running with carefully structured progression. Exercises become more dynamic, incorporating balance and proprioceptive challenges. Many patients return to full activities during this phase.
Return to activity phase (weeks 12+): Gradual return to desired activities continues, with ongoing maintenance exercises. Most patients can return to full activity within 3-4 months of consistent therapy, though some require longer depending on initial severity.
Important note: This timeline assumes consistent adherence to a home exercise program and appropriate activity modification. Patients who perform exercises only during therapy sessions typically experience slower progress. Conversely, highly motivated patients who diligently perform home exercises often progress faster.
Success Rates and Clinical Evidence
The evidence supporting physical therapy for patellofemoral syndrome is compelling. Research from PubMed’s extensive database demonstrates that approximately 70-90% of patients with patellofemoral syndrome improve significantly with conservative physical therapy treatment. A landmark study in the American Journal of Sports Medicine found that supervised physical therapy resulted in clinically meaningful pain reduction in 82% of participants.
Hip-focused interventions show particularly strong evidence. Multiple randomized controlled trials demonstrate that programs emphasizing hip strengthening produce superior outcomes compared to knee-focused exercises alone. This finding has transformed treatment approaches, with modern physical therapy increasingly emphasizing the kinetic chain rather than isolated knee treatment.
Research published by the Journal of Orthopedic & Sports Physical Therapy shows that comprehensive programs addressing multiple impairments (strength, flexibility, movement patterns) outperform single-component interventions. The evidence suggests that individualized assessment and targeted treatment based on specific deficits yields the best outcomes.
Long-term follow-up studies indicate that patients who complete physical therapy and maintain exercise programs experience sustained improvement. Importantly, physical therapy success rates remain high even for patients with chronic patellofemoral pain lasting years before treatment initiation, suggesting it’s never too late to benefit from appropriate rehabilitation.
Comparative effectiveness studies demonstrate that physical therapy produces outcomes comparable to or superior to surgery for most patients, with significantly fewer risks and faster recovery. This evidence supports physical therapy as the gold standard first-line treatment.
When to Consider Additional Treatment
While physical therapy successfully resolves patellofemoral syndrome in the vast majority of cases, some patients require additional interventions. Knowing when to explore supplementary treatments is important for optimizing outcomes.
Persistent pain after adequate physical therapy: If you’ve completed 8-12 weeks of consistent, high-quality physical therapy without meaningful improvement, further evaluation is warranted. This might indicate a different underlying condition requiring different treatment or additional diagnostic imaging.
Imaging-based findings: If imaging studies (X-rays or MRI) reveal significant cartilage damage or other structural abnormalities, your orthopedic specialist might recommend additional interventions. However, it’s important to remember that imaging findings don’t always correlate with symptoms—many asymptomatic individuals have abnormal imaging.
Injections: Some patients benefit from corticosteroid injections into the knee joint or surrounding structures. These can provide pain relief allowing more aggressive physical therapy participation. Hyaluronic acid injections may also be considered, though evidence for their effectiveness is mixed.
Surgical intervention: Surgery is rarely necessary for uncomplicated patellofemoral syndrome. Arthroscopic procedures like lateral retinacular release or tibial tuberosity transfer are reserved for specific anatomical abnormalities unresponsive to conservative treatment. Surgery should only be considered after exhausting conservative options and confirming structural abnormalities that specifically explain your symptoms.
Many patients benefit from combining physical therapy with complementary approaches. Gait analysis using video technology or force plate analysis can provide objective data guiding therapy. Running-specific physical therapy programs incorporate treadmill analysis and real-time feedback. Some patients find benefit in red light therapy near me as an adjunctive treatment for inflammation management.
Preventing Recurrence and Maintaining Long-Term Health
Successful recovery from patellofemoral syndrome requires ongoing attention to the factors that caused the condition initially. Recurrence is common among patients who discontinue exercise programs after pain resolution, making prevention crucial.
Maintenance exercise programs: Continuing strengthening exercises at reduced frequency (typically 2-3 times weekly) maintains the muscular adaptations developed during therapy. You needn’t perform the intensive programs required during active treatment, but consistent maintenance prevents deconditioning and recurrence.
Training principles: Follow evidence-based training principles to prevent excessive knee stress. Gradually increase training volume and intensity—the “10% rule” suggests increasing weekly training load by no more than 10%. Include adequate recovery days, vary training activities to distribute stress across different tissues, and incorporate cross-training to maintain fitness while reducing repetitive knee stress.
Footwear assessment: Proper running shoes or activity-specific footwear significantly influences patellofemoral joint loading. Consider gait analysis at a specialty running store or with your physical therapist to ensure appropriate footwear for your biomechanics. Worn-out shoes should be replaced before they contribute to movement dysfunction.
Periodic reassessment: Returning to your physical therapist annually or when training volume increases allows early identification of emerging imbalances. Addressing minor issues promptly prevents progression to symptomatic patellofemoral pain.
Activity modification: Continuing to avoid activities that previously aggravated your knee during the early recovery phase remains important. However, gradual, progressive exposure to these activities as strength improves prevents the fear-avoidance patterns that can develop with chronic pain.
Some athletes benefit from periodic coaching or form analysis to ensure they’re maintaining proper movement patterns. Others find value in understanding therapy costs and planning for periodic professional guidance to maintain optimal biomechanics.
Frequently Asked Questions
How long does physical therapy for patellofemoral syndrome typically take?
Most patients require 8-12 weeks of consistent physical therapy to achieve significant improvement, though some require longer. The timeline depends on symptom severity, how long you’ve experienced pain, and your adherence to home exercises. Attending therapy sessions alone, without performing home exercises, typically extends recovery significantly.
Can I return to running while undergoing physical therapy?
Yes, most patients can return to running during physical therapy, but progression must be carefully managed. Your therapist will provide specific guidelines for run-walk intervals, distance progression, and frequency. Returning too quickly or progressing too aggressively is a common cause of setback and should be avoided.
Do I need imaging studies (X-rays or MRI) to diagnose patellofemoral syndrome?
No, patellofemoral syndrome is typically diagnosed clinically based on your symptoms and physical examination findings. Imaging studies are reserved for cases not responding to conservative treatment or when other conditions are suspected. Many asymptomatic individuals have imaging abnormalities, making imaging unnecessary for straightforward cases.
Is patellofemoral syndrome permanent?
Patellofemoral syndrome is not inherently permanent. With appropriate physical therapy addressing underlying biomechanical issues, most patients achieve lasting pain resolution. However, returning to previous movement patterns or training errors can cause recurrence, emphasizing the importance of maintaining exercises and following training principles.
Can weight loss help patellofemoral syndrome?
Yes, weight loss can reduce patellofemoral joint loading and may help reduce symptoms. However, weight loss alone without addressing underlying biomechanical dysfunction is often insufficient. Combining appropriate physical therapy with gradual, healthy weight loss when applicable provides optimal outcomes.
What’s the difference between patellofemoral syndrome and patellofemoral pain?
These terms are essentially synonymous. “Patellofemoral syndrome” and “patellofemoral pain” both refer to pain around the kneecap related to altered patellar mechanics. The condition is also called “runner’s knee” or “anterior knee pain,” though it affects people beyond runners.
Should I wear a knee brace for patellofemoral syndrome?
Knee braces can provide symptom relief and proprioceptive feedback during early treatment, potentially allowing increased activity participation. However, evidence suggests braces work best as temporary adjuncts during physical therapy rather than long-term solutions. Relying on braces without addressing underlying deficits can lead to muscle atrophy and prolonged recovery.
Is surgery necessary if physical therapy doesn’t help?
Surgery is rarely necessary for patellofemoral syndrome. Before considering surgery, ensure you’ve completed adequate physical therapy (12+ weeks) with a skilled therapist, performed a diligent home exercise program, and addressed all modifiable factors. Imaging confirmation of specific structural abnormalities explaining your symptoms is essential before surgical consideration.